As a professional volleyball player for 10 years, I won’t lie, knee pain was something that plagued my career as I got older.
Knee pain presented at various intensities over the years in my career and is something that I see in the clinic daily as a Registered Physiotherapist. So if you are experiencing knee pain, know that you are not alone. In this article I will be focusing on one cause of knee pain that many weekend warriors and professional athletes alike may experience, Patellofemoral Pain Syndrome (PFPS).
Patellofemoral Pain Syndrome (PFPS), is a frequent musculoskeletal complaint that affects the knee joint. PFPS can arise from various intrinsic and extrinsic factors. Several biomechanics, anatomical, and physiological mechanisms are thought to contribute to the development of PFPS.1
Treatment and rehabilitation for PFPS can be challenging, the therapy approach should be individualized according to the underlying cause and severity of the symptoms. Non-surgical interventions such as exercise therapy, patellar knee bracing, physical therapy, and pharmacotherapy are the first line of treatment for PFPS.1

Confused, or still unsure what this condition is? don't worry!
I aim to provide you with a comprehensive overview of PFPS, aswell as and review some options to help manage symptoms recommended by the 2021 Clinical Practice Guidelines published by the Journal of Orthopaedic Sports and Physical Therapy.
What is Patellofemoral Pain Syndrome?
 Patellofemoral Pain Syndrome is a common musculoskeletal-related condition that is characterized by the insidious onset of poorly defined pain localized around the anterior retro patellar and/or peripatellar region of the knee. The onset of symptoms can be slow or develop quickly, with worsening pain typically presenting when lower limb loading (running, squatting, prolonged positioning, stairs, jumping).1
Patellofemoral Pain Syndrome is a common musculoskeletal-related condition that is characterized by the insidious onset of poorly defined pain localized around the anterior retro patellar and/or peripatellar region of the knee. The onset of symptoms can be slow or develop quickly, with worsening pain typically presenting when lower limb loading (running, squatting, prolonged positioning, stairs, jumping).1
What is the incidence of Patellofemoral Pain Syndrome?
Prevalence ranges from 3% to 85% of the population suffering from idiopathic knee pain (AKP) or PFPS and its associated diagnosis, with the prevalence of 25% being the most frequently cited. This represents between 1.5% and 7.3% of all patients seeking medical care.1
What demographic most often suffers from PFPS?
Patellofemoral Pain Syndrome can occur at any point during our life span, those affected range from from young children to older sedentary adults. Two groups have ben reported to have the highest incidence of PFPS, those between 12 and 19 years of age, and those between 50 and 59 years old.1
Will PFPS go away on it's own?
Patellofemoral Pain Syndrome is not a self limiting condition. Meaning that it's unlikely the condition will resolve on its own. Prevalence of PFPS was previously considered a common condition in adolescence that would eventually resolve over time. However 50%-56% of patients report persistent knee pain two years after their initial diagnosis. This can have a substantial impact on the quality of life and burden of living with PFPS such as loss off of physical function, loss of self identity, pain-related confusion and fear, and concern for the future.1

How do you know if you have PFPS?
Systematic reviews have concluded the PFPS symptoms produced by functional tasks such as running, squatting, stair climbing and sitting with flexed knees is currently the best indicator of PFPS. 1
Quadricep atrophy is a common finding in individuals with PFPS, but only when assessed by imaging. The atrophy is consistent across the three different vasti musculature and is not isolated to only the vastus medialis oblique musculature. Quadriceps inhibition of roughly 18% was also found in those suffering from PFPS. Suggesting that a loss of quadriceps strength is a contributing factor to PFPS.1
Furthermore, people with PFPS show weakness of the hip abductors, extensors and external rotators. Rate of force development of the hip abductors and extensors is also reduced in people with PFPS. However there is a strong possibility that hip weakness is a result of PFPS and not a direct cause of PFPS.1
PFPS Treatment and Therapy
 The best supported evidence suggests that a combined intervention of exercise therapy consisting of knee targeted and knee/hip targeted exercise, combined with foot orthosis, patellar knee bracing, patellar mobilization and/or biofeedback for the treatment of PFPS.1
The best supported evidence suggests that a combined intervention of exercise therapy consisting of knee targeted and knee/hip targeted exercise, combined with foot orthosis, patellar knee bracing, patellar mobilization and/or biofeedback for the treatment of PFPS.1
Exercise therapy typically consists of knee and/or hip-targeted exercises performed in weight bearing and non weight bearing positions, or both.1
When the individual combines knee targeted exercises with hip targeted exercises short term, medium term and long term outcomes all improve. Hip targeted exercises may prove to be superior to knee targeted exercises in the early stages of PFPS as they are typically tolerated better and can still have a positive outcome of PFP without targeting the knee.1
Individuals should therefore include exercise therapy combined with hip and knee targeted exercises in the treatment of PFP to reduce pain and improve self reported outcomes.1
Knee dominant / hip and knee dominant exercises which may prove useful in the treatment of PFPS include:
- Lying straight leg raise or for increased difficulty seated straight leg raise
- Terminal knee extensions or for increased difficulty seated leg extensions
- Wall sit or for increased difficulty single leg wall sit
- Side lying leg raise or for increased difficulty side plank plus leg raise
- Banded skater strides, or for increased difficulty RNT step up

Watch my most recent vlogs with Bauerfeind Canada HERE for an overview on treatment options and visual examples of the key exercises!
Bracing for Patellofemoral Pain Syndrome
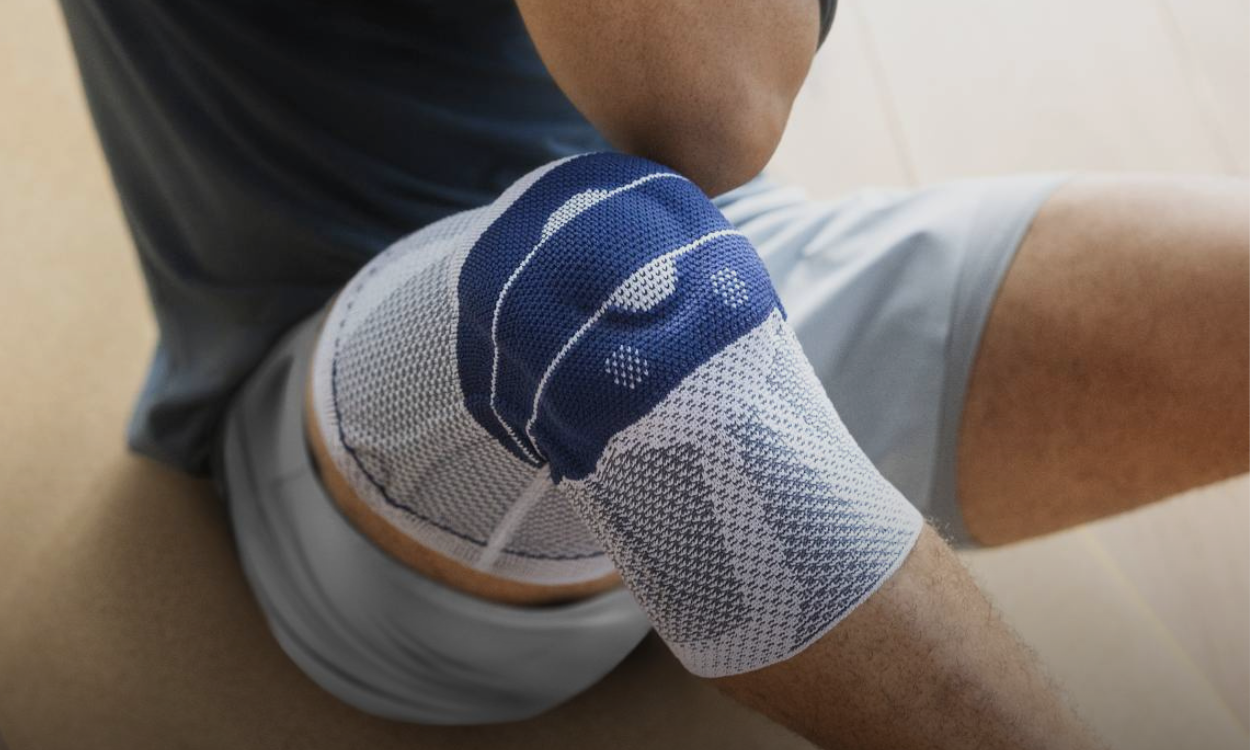
Bauerfeind has conducted observational studies with positive results using the GenuTrain P3 knee brace in regards to improvements in joint stability, reduction in self reported pain, and subjective improvements in mobility during daily activities.
Key features of the GenuTrain P3 include:
- Compressive Train knit material (20-30 mm HG)
- Lateral/medial rigid stays to improve joint stability
- An adjustable corrective strap to aid in reduction in lateral drifting of the patella
Using a brace such as the GenuTrain P3 as a way to improve an individual’s tolerance (reduction in pain) or ability to perform strength training activities (improvements in joint stability) would therefore serve as a positive adjunct in their rehab journey.
Learn More about the GenuTrain® P3 knee brace here!
So to sum it all up...
Patellofemoral Pain Syndrome (PFPS) is a common knee condition that can be caused by a variety of factors. It can lead to pain and discomfort in the anterior knee region, limiting daily activities and sports performance. Diagnosis and treatment of PFPS can be challenging, as the underlying causes and contributing factors can vary greatly from person to person. The best supported evidence in the treatment of PFPS involves a combination of hip and knee targeted exercises. The use of a knee brace can serve as a positive adjunct to treating PFPS as it may improve an individuals pain levels, improve joint stability and improve their ability to perform daily activities!
Please consult your physician for personalized medical advice. Always seek the advice of a physician or other qualified healthcare provider with any questions regarding a medical condition.
_____________________________________________________________________
References:
1. Illy R, Barton CJ, Bolga LA, Scalzitti DA, Logerstedt DS, Lynch AD, Snyder-Mackler LS, Mcdonough CM. Clinical Practice Guidelines Linked to the International Classification of Functioning, Disability and Health From the Academy of Orthopaedic Physical Therapy of the American Physical Therapy Association. J Orthop Sports Phys Ther. 2019;49(9):CPG1-CPG95.